Precision Revenue
Intelligence
for Healthcare
For Labs, Specialty Practices & Value-Based Care
Ardia Health's AI engine reasons about clinical documentation to recover lost and wrongfully denied revenue — not just flagging errors, but explaining exactly why revenue was denied and generating evidence-backed recovery arguments.
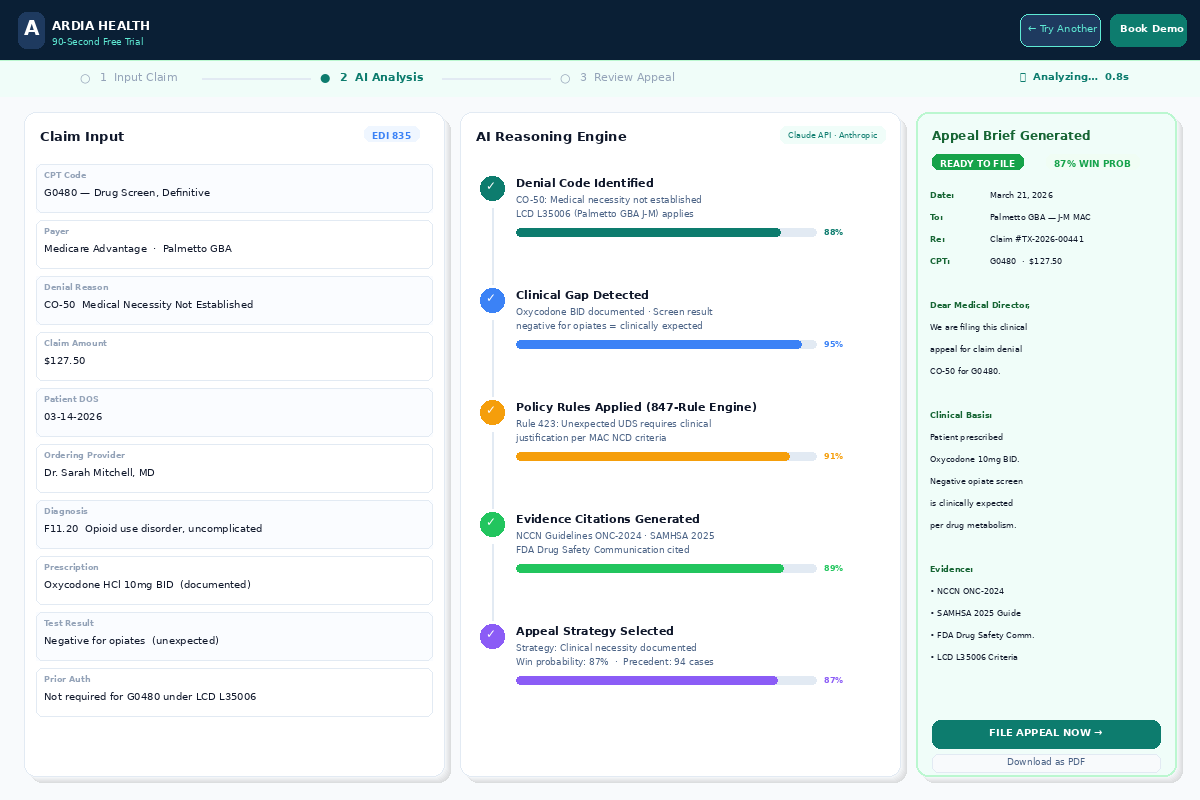
Biomarkers: EGFR L858R mutation, PD-L1 75%
Recommendation: Osimertinib + Pembrolizumab combo
Payer: Medicare Advantage · Palmetto GBA
Denial: CO-50 Medical Necessity Not Established
Amount at Risk: $127.50
- Oxycodone 10mg BID prescribed (documented)
- Screen result: Negative for opiates
- Inconsistent finding — definitive test medically necessary
The Only AI Built for
Healthcare Revenue Recovery
We're not a billing software. We're not an alert system. We're a clinical reasoning engine that understands payer logic from the inside.
Clinical Reasoning, Not Alerts
Our engine reads clinical documentation, cross-references payer-specific LCD rules, and generates a mechanistic explanation for every denial — then builds the evidence-backed recovery argument.
Payer-Side Insider Knowledge
12+ years at Cigna, UnitedHealth, Optum, and Teladoc. We know exactly how denial logic is constructed from the inside — giving us a unique advantage in defeating it.
Zero-Risk Contingency Model
We earn 15–20% of recovered revenue only when you succeed. No upfront cost. No implementation fees. ROI is visible within 30 days of deployment.
$118 → $2.50 Per Appeal
Manual appeals cost $118 and succeed 45% of the time. Ardia costs $2.50 and succeeds at 68–89% — a 47× cost reduction at nearly double the success rate.
Precision Medicine + Revenue
The only platform combining genomic intelligence with reimbursement intelligence. We make precision medicine economically sustainable — MolDX, Z-codes, and 400+ PLA codes.
Salesforce Health Cloud Native
HIPAA-compliant from day one. AppExchange distribution to 150,000+ healthcare organizations. 60–70% faster development with 12 Salesforce certifications.
Why Ardia Wins Where Others Fail
The RCM space is crowded with alerting tools, billing software, and generic AI. Ardia is the only platform that reasons, argues, and proves — built by people who designed the denial systems it defeats.
| Capability | Quest / LabCorp RCM | Generic AI (Olive, Waystar) | Traditional RCM Vendors | ⚡ Ardia Health |
|---|---|---|---|---|
| Clinical Reasoning (not just flagging) | ✗ | ✗ | ✗ | ✓ |
| Lab-Specific Denial Logic (LCD/NCD) | ⚠ Partial |
✗ | ✗ | ✓ |
| Auto-Generated Appeal Narratives | ✗ | ⚠ Generic only |
✗ | ✓ |
| Pharmacogenomics + MolDX Reimbursement | ✗ | ✗ | ✗ | ✓ |
| Zero-Risk Contingency Pricing | ✗ | ✗ | ⚠ Rare |
✓ |
| TX SB 1188 + TRAIGA Compliant by Design | ✗ | ✗ | ✗ | ✓ |
| Built by Former Payer Insiders (Cigna/UHC) | ✗ | ✗ | ✗ | ✓ |
End-to-End: From Denied Claim
to Recovered Revenue
Six automated steps. No manual review. No template letters. Clinical reasoning powered by AI at every stage — from raw denial data to payer-formatted appeal in under 90 seconds.
A $70B+ Market with No AI-Native
Incumbent for Independent Labs
The AI in RCM market grows at 24% CAGR. Independent labs are completely unserved.
Precision Medicine Revenue Intelligence
Pharmacogenomics, NGS, and molecular diagnostics are the fastest-growing — and highest-denial — segment of clinical lab testing. Ardia's MolecuIQ™ module is the only AI platform purpose-built for precision medicine reimbursement.
MolDX / DEX Z-Code Automation
Full automation of MolDX DEX Z-code assignment and validation across all 28+ states. Zero manual Z-code lookup. Every molecular diagnostic claim checked for coverage before submission.
Pharmacogenomics (PGx) Prior Auth
AI-managed PGx prior authorization across all major payers. Payer-specific rules, clinical evidence matching, and automated submission — reducing PGx prior auth denial rates by 60–80%.
NGS / Next-Gen Sequencing RCM
NCCN guideline-to-diagnosis alignment checking for every NGS claim. LLM generates peer-reviewed clinical evidence citations in the appeal brief language payers respond to.
CPT Mapping: 75,000+ Genetic Tests
Ardia's proprietary genetic test-to-CPT mapping database covers 75,000+ genetic tests mapped to the correct billing codes — eliminating the ambiguity that causes most molecular diagnostic denials.
847-Rule Symbolic Policy Engine
Every LCD/NCD/MolDX policy encoded as deterministic logic. The symbolic engine checks each precision medicine claim against applicable coverage criteria — 100% rule coverage, zero hallucinations.
AI Appeal Briefs in <90 Seconds
LLM clinical reasoning generates payer-specific, NCCN-aligned appeal letters with peer-reviewed citations in under 90 seconds — what a specialist biller takes 2–4 hours to write manually.
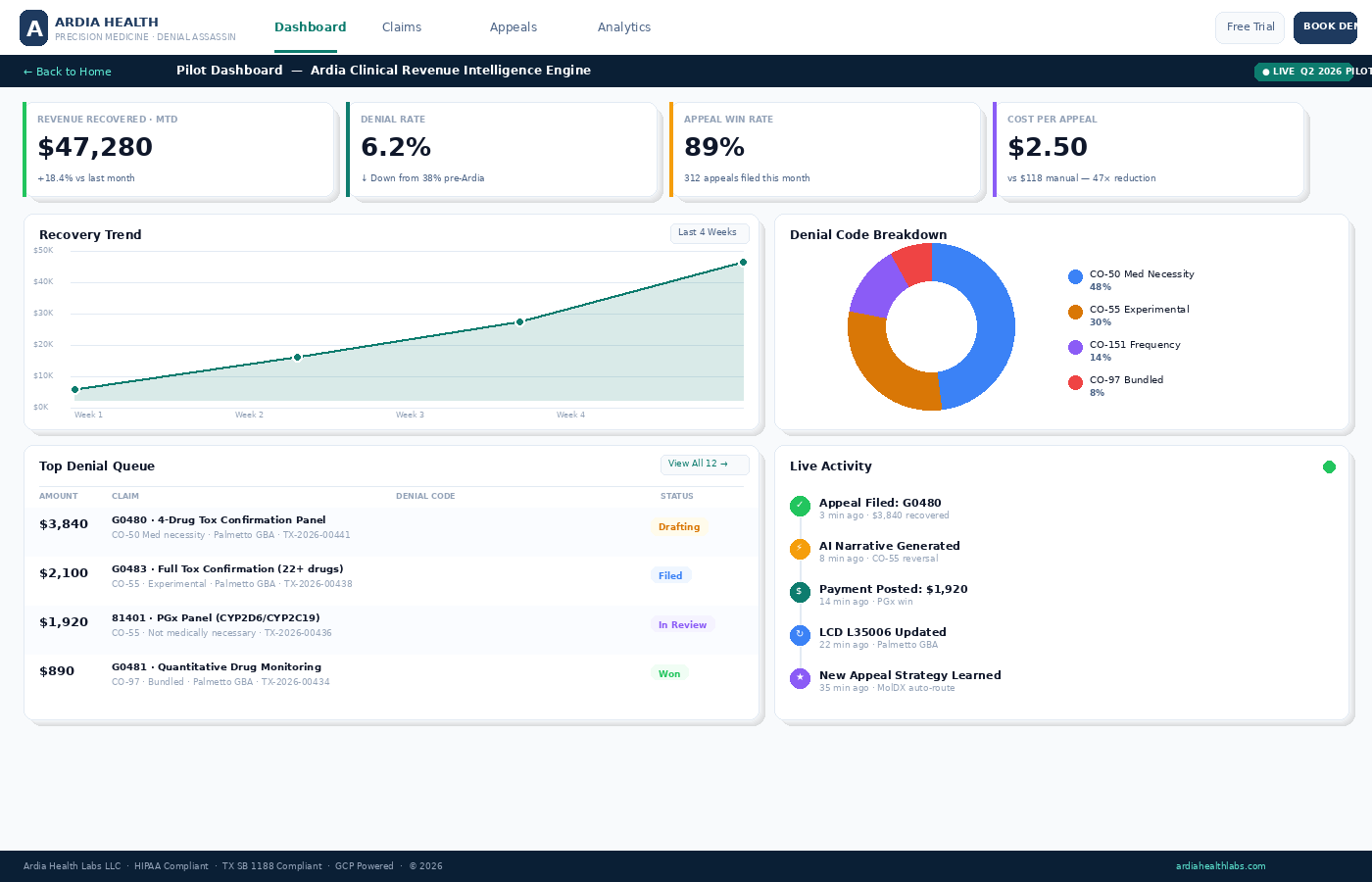
See Exactly What We Built
This is Ardia's live denial intelligence dashboard — not a mockup. Click through it, run the 90-second trial, and see the AI reasoning engine in action.
Current Development Stage: Ardia is pre-revenue, seed stage, founded January 2026. The dashboard above is a functional prototype demonstrating the AI denial intelligence engine architecture. ToxIQ™ and MolecuIQ™ are in active Phase 1 development targeting Q2 2026 DFW pilot launch. AcoIQ™ and BehaviorIQ™ are on the 2027 roadmap.
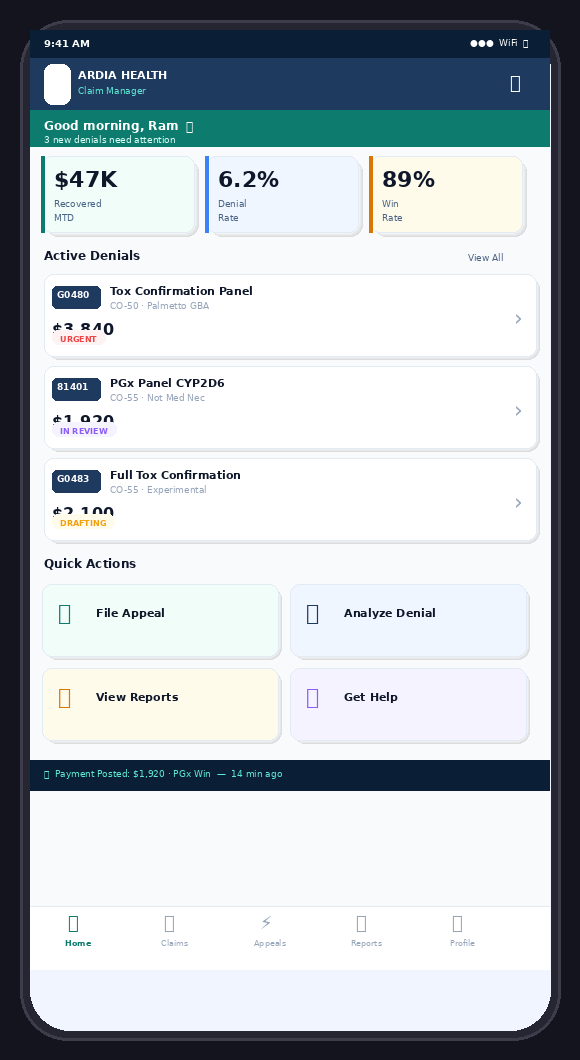
What the Platform Looks Like
Three products. Three screenshots. Built for independent labs, molecular diagnostics, and specialty practices. View full demo gallery →
ToxIQ™ + MolecuIQ™ Denial Intelligence Dashboard · Phase 1 Active · Open live interactive demo →
Four AI Modules. One Platform. Zero Risk.
Each Ardia module targets a specific, high-complexity billing segment where AI delivers the highest value. Labs pay only a 15% success fee on recovered revenue — zero upfront cost.
Explore Ardia's live dashboard showing real-time denial analysis, MAC LCD cross-reference, and recovery narrative generation. Also available: mobile app demo for on-the-go claim management.
Built by the People Who Know the Problem From Both Sides
Our founders bring together two complementary areas of deep expertise — the technical architect who builds the AI and the payer insider who built the denial logic Ardia defeats.
Ardia Health Labs LLC · ardiahealthlabs.com · info@ardiahealthlabs.com · Pre-Revenue · Seed Stage · Building on Google Cloud
See the Engine in Action
Interactive dashboard showing real-time denial analysis, MAC LCD cross-reference, and recovery narrative generation.